 It has been just over a year since I was diagnosed and operated on for colon-rectal cancer. Fortunately the cancer (stage I) was discovered early. It was revealed after I had my first colonoscopy at age 51. I had several more tests to determine the extent and location of the cancer. The doctors determined that the cancer was located just a few centimeters from my sphincter muscles. Luckily my surgeon believed he could save my sphincter and I would not require a permanent colostomy pouch. Instead I would have a temporary ileostomy bag. After I healed from the surgical removal of my rectum, the ileostomy would be taken down and I would be hooked back up “normally” again.
It has been just over a year since I was diagnosed and operated on for colon-rectal cancer. Fortunately the cancer (stage I) was discovered early. It was revealed after I had my first colonoscopy at age 51. I had several more tests to determine the extent and location of the cancer. The doctors determined that the cancer was located just a few centimeters from my sphincter muscles. Luckily my surgeon believed he could save my sphincter and I would not require a permanent colostomy pouch. Instead I would have a temporary ileostomy bag. After I healed from the surgical removal of my rectum, the ileostomy would be taken down and I would be hooked back up “normally” again. On November 13th 2009, I had my rectum removed at Kaiser Permanente Hospital in San Francisco. The surgery went well but I had a number of complications over the next several months dealing with an infection and abscess. I was in and out of the hospital a several of times. I spent close to a total of four weeks in the hospital between November and January. For the next 5 months I had an ileostomy bag hanging from the right side of my belly. The end of my small intestines was pulled through my abdominal wall so that waste could be discharged without passing through my healing colon. The care and management of this was time consuming and required lots of fidgety work. It was not as uncomfortable as I feared but it was really bizarre to have a piece of my insides hanging out. Finally in mid April I had my last operation to restore my colon to “normal”.
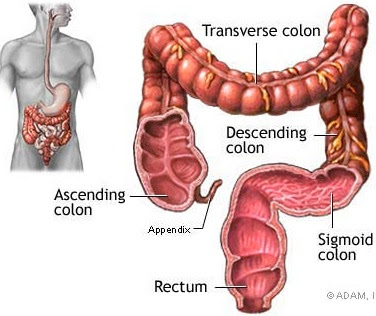
On November 13th 2009, I had my rectum removed at Kaiser Permanente Hospital in San Francisco. The surgery went well but I had a number of complications over the next several months dealing with an infection and abscess. I was in and out of the hospital a several of times. I spent close to a total of four weeks in the hospital between November and January. For the next 5 months I had an ileostomy bag hanging from the right side of my belly. The end of my small intestines was pulled through my abdominal wall so that waste could be discharged without passing through my healing colon. The care and management of this was time consuming and required lots of fidgety work. It was not as uncomfortable as I feared but it was really bizarre to have a piece of my insides hanging out. Finally in mid April I had my last operation to restore my colon to “normal”. This so called “normal” was a totally new reality. One does not usually think about their rectum and its function. I learned that the purpose of the rectum is to be a temporary holding area for your poop. When it fills up, it sends a signal to your brain telling you it is time to go. If all is well, you don’t think about it more then once or twice a day. For the first month out of the hospital I found myself going 60 to 80 times a day. My colon was doing its job of pushing food waste along (peristaltic waves). But there was no rectum at the end to collect it. I felt like a rabbit pooping little pellets all the time. Although the surgeon has shaped the last part of my colon to act like a small rectum (transverse coloplasty pouch), I was going to have to train it to act like one.
This so called “normal” was a totally new reality. One does not usually think about their rectum and its function. I learned that the purpose of the rectum is to be a temporary holding area for your poop. When it fills up, it sends a signal to your brain telling you it is time to go. If all is well, you don’t think about it more then once or twice a day. For the first month out of the hospital I found myself going 60 to 80 times a day. My colon was doing its job of pushing food waste along (peristaltic waves). But there was no rectum at the end to collect it. I felt like a rabbit pooping little pellets all the time. Although the surgeon has shaped the last part of my colon to act like a small rectum (transverse coloplasty pouch), I was going to have to train it to act like one.Fortunately, a friend of a friend came to may aid. He had a similar operation a couple years back and had a strategy that worked for him. He had found a bowel-training program that worked with a combination of Metamucil (psyllium, a dietary fiber supplement) and antidiarrheal medications such as Lomotil or Immodium.
 If you are interested, the bowel-training program can be found HERE. My new regimen consists of starting off the day with a large meal. I then stay close to the bathroom for a couple of hours. When I am ready to go out I take an Immodium or two. Lunch and dinner consists of very, very small amount of food - no more than a cup or two in size. It is followed by a very concentrated shot of 3 teaspoons of Metamucil dissolved in a couple ounces water. I don’t have any food restrictions. However, I have learned some foods are no longer easy to digest, especially beef and corn for example. Other than at breakfast, I can’t have hot liquids such as coffee or soup. Rich and sweet foods (cakes, cookies, chocolate, etc.) also are limited to mornings. Some days are a real challenge and I can’t go more than a few hours without thinking about and physically clenching and squeezing my butt muscles to hold it all in.
If you are interested, the bowel-training program can be found HERE. My new regimen consists of starting off the day with a large meal. I then stay close to the bathroom for a couple of hours. When I am ready to go out I take an Immodium or two. Lunch and dinner consists of very, very small amount of food - no more than a cup or two in size. It is followed by a very concentrated shot of 3 teaspoons of Metamucil dissolved in a couple ounces water. I don’t have any food restrictions. However, I have learned some foods are no longer easy to digest, especially beef and corn for example. Other than at breakfast, I can’t have hot liquids such as coffee or soup. Rich and sweet foods (cakes, cookies, chocolate, etc.) also are limited to mornings. Some days are a real challenge and I can’t go more than a few hours without thinking about and physically clenching and squeezing my butt muscles to hold it all in.Things that are a challenge:
- Can’t take for granted that I can always control when I poop.
- If I don’t stick to my eating and Metamucil program, there are unpleasant consequences. Gone are the days of eating whenever and whatever I want.
- Eating, drinking, sex, going out to a movie or a play are no longer spontaneous activities. They now require planning, organizing, and preparation.
- Wherever I go, I need to carry a bag of supplies: Metamucil, Immodium, spare underwear, extra toilet paper and underwear pads.
- Keeping a sense of humor when my body betrays me.
 When I start to get overwhelmed or depressed about the situation, I try to remember the positive outcomes:
When I start to get overwhelmed or depressed about the situation, I try to remember the positive outcomes:- I am alive, active and productive. I am working part-time. I can travel (we spent the month of August in Scandinavia). I started running again.
- I didn’t need radiation or chemotherapy or a permanent colostomy bag.
- The procedures didn’t make me impotent or have erectile dysfunction or urinary incontinence (all possible side effects).
- I have lost 15 pounds from my high point. My clothes fit better and friends say I look healthier. I would still like to lose 7 to 10 more pounds.
- I have the most wonderful and supportive husband. He has taken great care of me in a multitude of ways.
- The doctors, nurses and staff at Kaiser Permanente have been first rate. I could not have asked for a better health team.
Previous entries about my surgery and recovery: : 1, 2, 3, 4, 5.
9 comments:
Hello guydads
Thanks so much for sharing your story. I had a section of my colon removed in June of this year. I had a few complications but nothing like you did, and I was spared everything except the surgery.
I have struggled mightily with getting control of my bowels as well, and I too have been busy counting my blessings (nothing else to do while on the toilet). I have been following the advice of my doctors, which is basically 'be patient and it will get better', so I was thrilled to see your link to lowrectalcancer.com.
Very best of luck in your continued recovery.
Paul
Wow. Thanks for sharing such a personal experience. I'm sorry you had to go through any of it, but it's good to see that you can still highlight the positives in all of this.
There's no place for shame when it comes to colon cancer and it's refreshing that you would discuss all the gritty details so openly.
I wish you the very best possible recovery results.
Hey guys - hope you're having a good holiday! Thank you for sharing that story - certainly something I don't think about but I would guess that it's very good to know. I am glad you are still able to see positive aspects of your life and you do not give in to depression as so many would...and you're still sexy...hubba hubba...
I'm a 23+ years (and counting praise God) Colon Rectum Cancer (CRC) Survivor.
When I was diagnosed with Colon/Rectum Cancer (Also called Colorectal Cancer -CRC) over 23+ years ago, it would have been so comforting to have someone come beside me and share their journey. Someone to tell me, “I’ve been there and here’s what I can tell you from my experience.”
I know how hard it is but it gets better. It's our attitude and seeking to find ways to use what we experience in life. Sometimes it's one day at a time. I just started sharing my journing in a blog and hope to encourage others in doing so. Online world is so new to me. I've only discovered computers about a year ago and it has been so wonderful.
God bless,
Dee Dee
http://chatwithdeedee.wordpress.com/
My sister had ulcerative colitis and her large intestine removed less than a year ago and now her small intestine is doing the work. It hasn't been easy but she is finally feeling better. You are so lucky that you caught your cancer early. I know someone who had symptoms for a very short time and by the time they found it it was very advanced. He fought for three years but lost his fight last month. So happy you are doing so well. Please share thoughts on The Next family and add your blog to the comment.
thanks for this post. i'm so glad to come across your blog again. hope you're having a good new year. :)
You are very courageous. What you live with on a daily basis makes my aches and pains seem petty and inconsequential. Also make us realize that we should take nothing for granted, and be grateful for every day. Stay well.
Colon cleanse can eliminate toxins and waste from your colon, whereas the colon naturally cleans its self to. Even though, after the natural cleaning of the colon, some waste may still remain on the colon’s walls, and to get rid of such waste.
Gents, it's really sad to hear these stories. Honestly, without malice, doesn't this tell you that what you're engaged in (homosexuality) might be unnatural?
Yah Bless.
Post a Comment